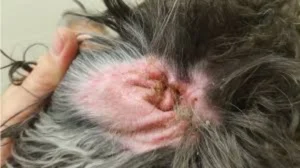
Ear Infections in Dogs: Causes, Symptoms & Treatment
Ear infections are among the most frequently reported reasons for veterinary consultations in India, yet they are also among the most commonly undertreated. A single course of ear drops may

Severe gastrointestinal illness can deteriorate quickly.
Vomiting, diarrhoea, hemorrhagic gastroenteritis (HGE), pancreatitis, and acute dehydration can lead to:
These changes can occur within hours.
In a city like Bengaluru, repeated hospital visits often mean long commutes, fragmented treatment, and long gaps between monitoring.
The VOSD GI Stabilisation Residency™ provides structured inpatient stabilisation under continuous supervision, delivered at VOSD IPD, Indiranagar, and managed under the VOSD Level of Care™. This is uninterrupted gastrointestinal intensive care designed for urban emergency medicine.
Since vomiting and diarrhoea appear suddenly and dramatically, pet parents often experience intense anxiety when they see:
Many spend sleepless nights watching symptoms and worrying about dehydration. The VOSD GI Stabilisation Residency™ replaces that uncertainty with continuous monitoring. Instead of waiting for the next appointment, parents know their dog is under supervision.
The GI Stabilisation Residency™ is a 48-96-hour structured inpatient stabilisation protocol designed for dogs experiencing acute gastrointestinal crises.
It provides:
Unlike routine admission, the Residency follows a defined clinical pathway with documented monitoring cycles and recovery milestones. This structured approach helps stabilise the patient safely and consistently.
Gastrointestinal illness can escalate quickly.
Vomiting and diarrhoea can cause:
In conditions like Hemorrhagic Gastroenteritis (HGE), deterioration may occur within 6-12 hours. When treatment occurs only during outpatient visits, there are long periods without monitoring. During these gaps:
Continuous monitoring reduces these risks.
Each Residency begins with a baseline evaluation.
This includes:
This baseline allows doctors to track response to treatment.
The first stage focuses on correcting dehydration and stabilising the patient.
Monitoring includes:
The goal is to restore hydration and reduce acute symptoms.
Once the patient stabilises, treatment focuses on improvement trends.
Monitoring includes:
These steps ensure stabilisation is sustained.
When vomiting and dehydration resolve, the program transitions toward recovery.
This includes:
Each patient receives written discharge instructions.
The GI Stabilisation Residency™ operates under the VOSD Level of Care™, a structured hospital management framework developed through VOSD’s large-scale clinical experience.
Across VOSD systems:
This institutional experience allows earlier recognition of complications and more precise stabilisation.
The GI Stabilisation Residency™ is delivered within the dedicated inpatient environment at VOSD IPD. This facility supports uninterrupted medical care.
This environment ensures treatment continuity during acute illness.
The GI Stabilisation Residency™ includes structured transparency for pet parents.
Each Residency provides:
Parents receive clear documentation of progress and next steps.
| Feature | Routine Admission | GI Stabilisation Residency™ |
| Monitoring | Periodic | Continuous observation |
| Duration | Undefined | Structured 48–96 hour protocol |
| Labs | As required | Scheduled reassessment |
| Escalation | Reactive | Built into the protocol |
| Parent Updates | Basic | Structured daily report |
| Discharge | Verbal advice | Written recovery roadmap |
Structured stabilisation reduces treatment variability.
Long-term medical care for critical and complex cases.
Medically supervised sterilization for high-risk animals.
Dedicated care for kidney-related conditions.
Specialized treatment for liver diseases.
Care for severe gastrointestinal disorders.
Controlled environment for contagious conditions.
Intensive monitoring and insulin therapy for diabetic crises.
Emergency treatment for poisoning and toxin exposure.
Remote consultations, second opinions, and ongoing case management.


info@vosd.in
Structured gastrointestinal stabilisation may be recommended when a dog has:
These conditions require stabilisation that cannot always be achieved through intermittent outpatient visits.
VOSD IPD serves pet parents across Bengaluru, including: Koramangala, Domlur, HAL, Ulsoor, and Whitefield. The facility is designed specifically for intensive veterinary care in urban settings.


Ear infections are among the most frequently reported reasons for veterinary consultations in India, yet they are also among the most commonly undertreated. A single course of ear drops may

Is your dog running a fever? Learn how to check dog temperature, identify tick fever symptoms, and when to seek emergency vet care, expert diagnosis at VOSD Advance PetCare™.
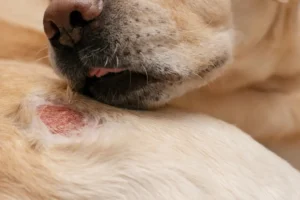
Is your dog scratching constantly? Learn causes, symptoms, and treatment of dog skin infections, allergies, hot spots, and hair loss, expert dermatology at VOSD Advance PetCare™.

Understand how parasites affect dogs, the warning signs to watch for, and how proper treatment and prevention can protect your pet.